Abstract
Covid infection is known to have a low fatality rate in young people and those without comorbidities. The classic triad of high temperature, new continuous cough, and loss of smell may not be present in all cases. Unusual presentations and initial negative Covid test can be detrimental in accessing treatment, leading to dangerous consequences in young people.
Case Presentation
This 27-year-old gentleman with no known comorbid conditions was unwell for two weeks before death. The symptoms were described as cold sweat and shivering. A Covid test from the local test center was negative. He was on symptomatic treatment with paracetamol and oral fluids. The patient went to local surgery three days before death and was refused an appointment. Two days later, he developed blue lips, shivering, blue fingertips followed by numbness of both legs. An ambulance was called. As the paramedics enter, the property patient walked down the steps and collapsed. Despite the best efforts of resuscitation, the patient sadly passed away. As the cause of death was unknown, a post mortem was conducted for Her Majesty’s Coroner.
On examination, both lungs appeared firm, heavy, and erythematous with dark patches. The right lung weighed 1600 gm, and the left lung weighed 960 gm. There was no macroscopically visible thrombus, pus, or thick mucus. No pleural effusion was present.
On microscopy, both lungs showed features of acute lung injury with diffuse alveolar damage, hyaline membranes, Type II pneumocyte hyperplasia, extramedullary, hematopoiesis, and inflammatory infiltrate of lymphocytes and plasma cells as well as multinucleated giant cells (Figure 1,2).
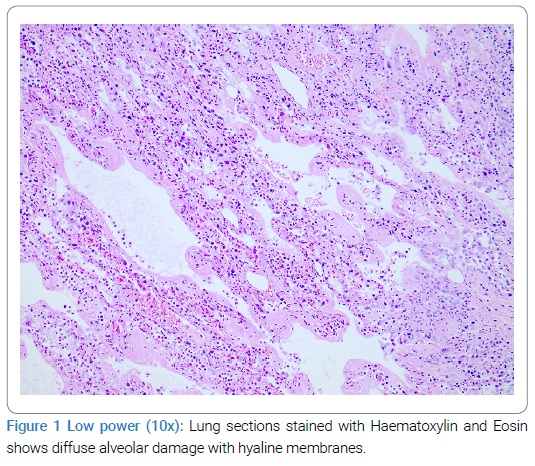
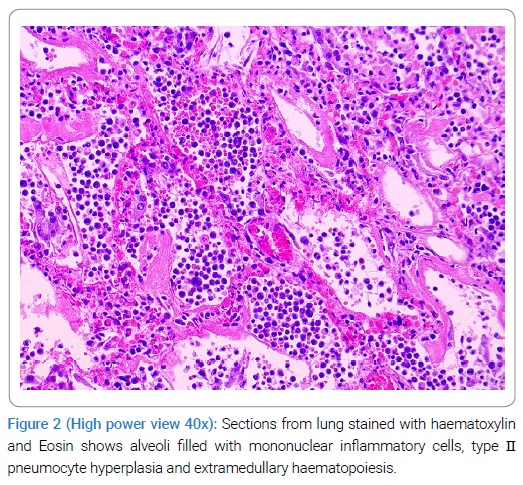
Another feature in histology was the presence of a thrombus in pulmonary blood vessels of small and medium-size (Figure 3).
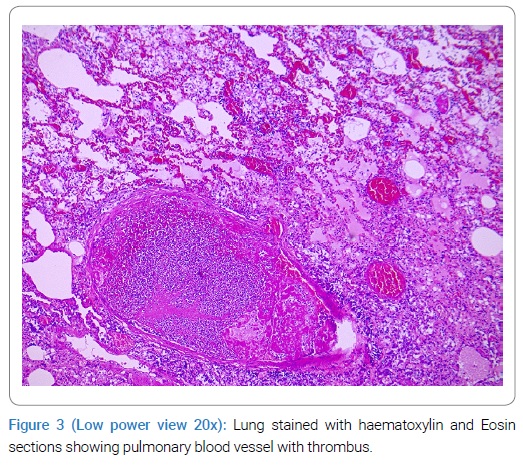
The heart on macroscopic examination was enlarged and weighed 600 gm. The valves and great vessels were normal. There was no evidence of infarction, rupture, or endocarditis. Coronary arteries were normal.
Kidneys on macroscopic examination were unremarkable. On microscopy, there was the presence of luminal microthrombi in the small vessels.
Liver on macroscopic examination weighed 2950 gm. Microscopy showed fatty change with microvesicular steatosis. No thrombosis or inflammation was seen in the liver (Figure 4).
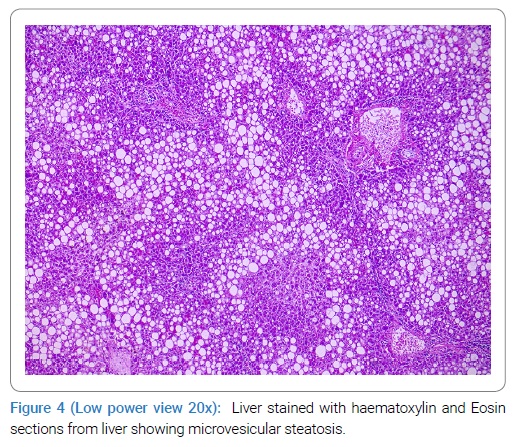
All other visceral organs were normal on macroscopic and histological examination.
A post-mortem Covid nasal swab done detected the presence of viral RNA.
Discussion
The post-mortem appearances are of untreated Covid pneumonia. Fibrin microthrombi is a constant finding in lungs and other organs in published cases of COVID [1]. The mechanism suggested is an immune triggered complement-mediated thrombotic microangiopathy. The clinical picture is not typical of disseminated intravascular coagulation [2]. Disproportionate tendency for thrombosis and the increased mortality rate is reported in young patients without comorbid conditions [3]. Microvesicular steatosis of the liver is also a common finding, even in the absence of any known liver conditions. The immune mechanism is postulated in the pathogenesis [4].
The sequence, degree, and rate by which an initial innate immune response is initiated vary from individual to individual. The infection in some people progress to microangiopathy, cytokine storm, and/or ARDS and proves fatal. The activation of immune cells, IL-6 and IL-1, are immune factors that are associated with ARDS. Various factors contribute to macrothrombosis and micro thrombosis in both the early and late stages of the disease [2].
The deceased had no known comorbid conditions associated with increased fatality from Covid. The clinical presentation was unusual as there was no classic triad of symptoms of high fever, continuous cough, loss of smell, or taste used to triage Covid diagnosis in a primary health care setting. As the classic symptoms were absent and the initial lab test was negative, the patient did not get the opportunity to be assessed in a medical facility.
This is also an eye-opener to educate people more on the warning signs of danger and seek medical attention.
Acknowledgments
The authors acknowledge support of H.M Coroner for the publication of this paper.
Author Contribution
Anu Gunavardhan and Muhammad Babar Aslam: Contributed equally to preparation, editing and revision of manuscript.
Ethical Approval
Consent from H.M Coroner was sought for publication of this article. No ethical Committee approval was required for this publication.
Conflict of Interest
The authors claim no conflicts of interest.
Keywords
Covid pneumonia; Thrombosis; Young; Mortality
Cite this article
Gunavardhan A, Aslam MB. Unexplained death in community diagnosed at post-mortem as Covid pneumonia. Clin Case Rep J. 2021;2(2):1–4.
Copyright
© 2021 Anu Gunavardhan. This is an open access article distributed under the terms of the Creative Commons Attribution 4.0 International License (CC BY-4.0).




